- Introduction to Subjective Methods
- Birth weight
- Body shape
- Weight and height
- Waist and hip circumference
- Introduction to Objective Methods
- Simple measures - stature
- Simple measures - weight
- Simple measures - circumference
- Simple measures - arm anthropometry
- Simple measures - skinfolds
- Simple measures - abdominal sagittal diameter
- Simple measures - head circumference
- Bioelectric impedance analysis
- Multi-component models
- Hydrostatic underwater weighing
- Air displacement plethysmography
- Hydrometry
- Whole body DEXA scan
- Near infrared interactance
- Whole body counting of total body potassium
- 3d photonic scan
- Magnetic resonance imaging (MRI) / Magnetic resonance spectroscopy (MRS)
- Total body electrical conductivity (TOBEC)
- Computed tomography (CT)
- Ultrasonography
- Introduction anthropometric indices
- Body mass index
- Fat and fat free mass indices
- Ponderal index
- Percentiles and Z-scores
- Anthropometry Video Resources
- Height procedure
- Protocol for measuring waist circumference
- Measuring hip circumference
- Weight and body composition procedure
Simple measures - arm anthropometry
Arm anthropometry is used as a proxy measure of body composition (e.g. muscularity, fat free mass and fat mass) by assessing the shape of the upper arm in both clinical and field settings.
Arm anthropometry includes:
- Upper arm length
- Mid upper arm circumference (MUAC)
- Triceps skinfold (TSF).
These measurements are used to derive the following indices of body composition:
- Arm muscle area (AMA)
- Arm fat area (AFA)
- Arm fat index (AFI)
Instrumentation
A non-stretchable insertion tape is typically used to assess MUAC and arm length. The tapes are generally graduated in millimetres.
Some tapes also have inbuilt MUAC cut off values to assess nutritional status and are colour coded (red indicates severe acute malnutrition, orange - moderate acute malnutrition, yellow - acute malnutrition and green - well nourished). Not all tapes include the colour orange.
These particular tapes vary according to the population under investigation (e.g. infants, children, adults or older adults).
If deriving the arm anthropometry indices, a skinfold caliper is used to assess the triceps skinfold (TSF).
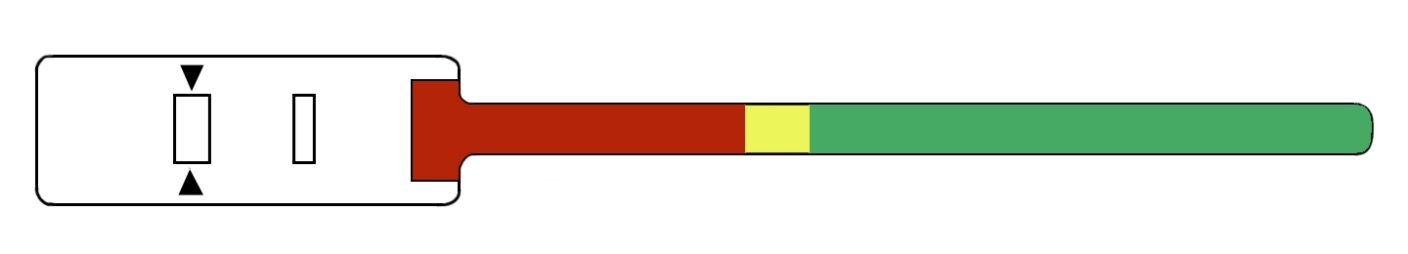
Figure 1 An insertion tape with three colour codings.
Source: UNICEF technical bulletin 13 MUAC
Procedure:
- The non-dominant arm is typically used to assess arm anthropometry. The arm of the participant requires to be bent at the elbow at a 90 degree angle.
- With the upper arm held parallel to the side of the body, the arm length between the bony protrusion on the shoulder (acromion) and the point of the elbow (olecranon process) is measured. The mid-point is marked between these anatomical landmarks.
- The upper arm circumference is taken at this point, while the participant’s arm hangs loosely by the side.
- The tape measure is snug around the upper arm but not too tight.
- The measurement is recorded to the nearest millimetre.
If deriving the arm anthropometry indices, the triceps skinfold (TSF) is also measured with a skinfold caliper at the same midpoint of the arm.
MUAC in isolation is commonly used in nutrition surveillance and screening programs to quickly assess nutritional status. Typically, it is used for the detection and referral of individuals with acute malnutrition.
Estimation of MUAC is important for assessing chronic energy deficiency, but it has also been found to be a useful screening tool for obesity, particularly in children and adolescents.
MUAC is also implemented to predict BMI categories. For instance, it is frequently used in older individuals or in hospitalised patients when weight combined with height, or arm-span or half-span cannot be derived.
MUAC can be used in combination with other arm anthropometry such as triceps skinfold (TSF) to derive the arm anthropometric indices arm muscle area (AMA), arm fat area (AFA), and arm fat index (AFI). These are used for the assessment of regional and total fat mass and fat free mass in resource-limited settings, in hospital settings (in acute disease) or field research settings, where current reference methods of body composition are not feasible.
These indices have been used to evaluate nutritional status and nutritional interventions in patients. Other applications include their use in the interpretation of nutritional status of populations with regard to normal reference curves in research settings.
Measurements of MUAC require very little data processing to derive final estimates of body composition. Estimates should be quality checked during data processing in the same manner as other health related variables, for example by checking for outliers and data entry errors.
MUAC is recorded in mm and this measure equals muscle + bone + fat, as shown in Figure 2.
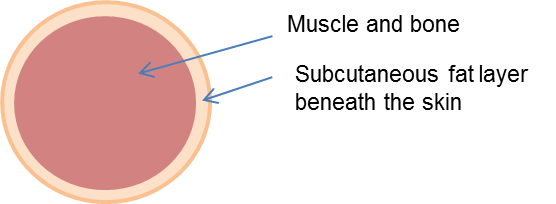
Figure 2 Illustration of components of a measure of mid-upper arm circumference.
Source: MRC Epidemiology Unit.
MUAC can be used to predict BMI to assess nutritional status (e.g. underweight and overweight) in different ages.
Typically
A MUAC of <235 mm -> BMI is likely to be <20 kg/m2
A MUAC of >320 mm -> BMI is likely to be >30 kg/m2
There are cut-off values for children, adults and older individuals, which correspond to BMI categories. Cut-offs are age, sex and population dependant.
Cut-offs in infants and children:
- Chaput et al. (2016)
- Craig et al. (2014)
- Mazıcıoğlu et al. (2010)
Cut-offs in adults:
- Ferro-Luzzi et al. (1996)
- James et al. (1994)
- Chakraborty et al. (2009)
- Bisai et al. (2009)
- Gartner et al. (2001)
Cut-offs in older individuals:
- Ismail et al. (1999)
- Tsai et al. (2010)
MUAC in the under five year old's, can also be interpreted by comparison against population standards (e.g. WHO standards for arm circumference by age; see www.who.int Source: [16])
Calculation of arm anthropometric indices
MUAC and TSF are converted from millimetres to centimetres.
The following are the most widely used equations assuming the arm has a cylindrical shape.
- Total upper arm area (TUA) = MUAC2 / (4*π)
- Arm muscle area (AMA) = [MUAC - (TS*π)]2 / (4*π)
- Arm fat area (AFA) = TUA - AMA
- Arm fat index (AFI) = (AFA / TUA)*100
Where MUAC and TSF are in centimetres and TUA (total upper arm area), AMA and AFA are in square centimetres and AFI as a percentage.
Equations containing correction factors for bone contributions (humerus) are also available.
The most widely used are reported by Heymsfield et al. (1982). These equations subtract mid-arm bone area (using the constant value of 10 cm2 in men and 6.5 cm2 in women) from the original equations on the basis that bone does not atrophy in proportion to muscle in severe wasting, and that the original equation tends to overestimate AMA when compared with CT values.
Arm circumference-for-age
The arm index, arm circumference-for-age is used as an alternative indicator of nutritional status when the collection of length/height and weight measurements is difficult, as happens in emergency humanitarian situations due to famine or refugee crises.
This index is expressed in percentiles (percentage of median) and can be assessed by the percentile point achieved by a child relative to the healthy children of that age and gender in the same population. Median is regarded as a reference value, and 3rd and 97th97th percentiles as thresholds to indicate abnormally low or abnormally high values.
Arm circumference-for-age index can also be expressed as Z-score derived by using the formula:
(Measured value – Average value in the reference population) / Standard deviation of the reference population
The WHO growth standards for arm circumference-for-age are used for interpretation in infants between 3 months and 5 years.
An overview of the arm anthropometry method is outlined in Table 1.
Strengths
- Inexpensive.
- Non-invasive.
- Can be measured without difficulty in almost any settings.
- Limited burden to participant.
- Limited burden to researcher in terms of collection and analysis.
- Requires no input by participant and as such no risk of respondent biases.
- Can be used when weight for height and BMI cannot be derived (e.g. due to oedema, ascites, curvature of the spine or immobility).
- Practical alternatives to BMI and current body composition methods to assess nutritional status in resource-poor settings.
- MUAC especially is a quick and easy measure when testing large groups, important during an emergency situation (e.g. acute malnutrition) or screening surveys.
- MUAC is better predictor of mortality in under five year old's when compared with weight-for-height and is subject to fewer errors than weight-for-height.
- MUAC is a good indicator of muscle mass and can be used as a proxy of wasting. It is also a good predictor of the risk of death.
- Arm anthropometric indices are useful for predicting fat mass and ranking individuals for fatness.
- Good agreement (despite over- or underestimation) between anthropometric arm muscle and fat area and the cross-sectional area measured by CT and ultrasound.
Limitations
- No agreement if MUAC cut-off values used for the assessment of obesity are required to be age-specific and population specific.
- No agreement for the interpretation of MUAC values for the assessment of undernutrition in children less than 6 months old, in adults and older adults. Cut-off values maybe population specific.
- AMA is a poor predictors of regional or total body FFM.
- Equations for AMA and AFA that contains correction factors for bone contributions (humerus) are not applicable in a paediatric population due to the greater variation in bone size.
- The value of arm muscle and fat area are proxies for lean and fat mass.
- The method relies on the following assumptions:
- The arm is cylindrical in shape
- The subcutaneous fat layer is evenly distributed around a circular core of muscle
- The triceps skinfold separates fat and lean components of the arm accurately and represents twice the thickness of subcutaneous fat in the arm.
- Population standards are not available for all the arm anthropometry measures.
- As growth affects changes in body composition, analysis adjustment for age and body size maybe required for the arm anthropometry indices.
- Arm anthropometry indices are poor predictors of regional or total fat free mass in children.
- Wrapping the measuring tape too tightly or too loosely could result in an erroneous estimate and observer variability.
Table 1 Characteristics of arm anthropometry methods.
| Consideration | Comment |
|---|---|
| Number of participants | Large |
| Relative cost | Low |
| Participant burden | Low |
| Researcher burden of data collection | Low |
| Researcher burden of coding and data analysis | Low |
| Risk of reactivity bias | No |
| Risk of recall bias | No |
| Risk of social desirability bias | No |
| Risk of observer bias | Yes |
| Space required | Low |
| Availability | High |
| Suitability for field use | High |
| Participant literacy required | No |
| Cognitively demanding | No |
Considerations relating to the use of the arm anthropometry method in specific populations are described in Table 2.
No guidelines currently exist for the measurement of individuals with physical disabilities, MUAC measurements may be misleading in cases where upper arm muscle might build up to aid mobility.
Table 2 Use of arm anthropometry methods in different populations.
| Population | Comment |
|---|---|
| Pregnancy | Suitable. |
| Infancy and lactation | Suitable, but not recommended for use among infants aged below 3 months due to lack of reliability data; For children aged 6-60 months, adjusting MUAC by calculating the Z-score or adjusting for height does not improve MUAC predictive value. Distraction techniques such as toys, bubbles help occupying the children during the measurement. |
| Toddlers and young children | Distraction techniques such as toys, bubbles help occupying the children during the measurement. |
| Adolescents | Suitable. |
| Adults | Suitable. |
| Older Adults | The mid-upper arm muscle area calculation may not be valid in obese or older individuals. |
| Ethnic groups | Suitable. |
| Other (e.g. Obesity) | The mid-upper arm muscle area calculation may not be valid in obese or older individuals. |
* TOBEC has been used mainly to monitor changes in body composition in women during pregnancy or lactation, in infants and in childhood obesity.
Refer to section: practical considerations for objective anthropometry
- Non stretchable tape measure and caliper if assessing triceps
- Data entry form in either paper or electronic form.
- Training of staff required
- Standard operating procedures for data collection.
- Standard operating procedures for data entry errors/extreme values/data cleaning.
- Toys (like bubbles) if measuring younger children
A method specific instrument library is being developed for this section. In the meantime, please refer to the overall instrument library page by clicking here to open in a new page.
- Bisai S, Bose K. Undernutrition in the Kora Mudi tribal population, West Bengal, India: a comparison of body mass index and mid-upper-arm circumference. Food and nutrition bulletin. 2009;30(1):63-7. Epub 2009/05/19.
- Chakraborty R, Bose K, Bisai S. Mid-upper arm circumference as a measure of nutritional status among adult Bengalee male slum dwellers of Kolkata, India: relationship with self reported morbidity. Anthropologischer Anzeiger; Bericht uber die biologisch-anthropologische Literatur. 2009;67(2):129-37. Epub 2009/09/11.
- Chaput JP, Katzmarzyk PT, Barnes JD, Fogelholm M, Hu G, Kuriyan R, et al. Mid-upper arm circumference as a screening tool for identifying children with obesity: a 12-country study. Pediatric obesity. 2016. Epub 2016/05/31.
- Chiba T, Lloyd DA, Bowen A, Condon-Meyers A. Ultrasonography as a method of nutritional assessment. JPEN Journal of parenteral and enteral nutrition. 1989;13(5):529-34. Epub 1989/09/01.
- Chomtho S, Fewtrell MS, Jaffe A, Williams JE, Wells JC. Evaluation of arm anthropometry for assessing pediatric body composition: evidence from healthy and sick children. Pediatric research. 2006;59(6):860-5. Epub 2006/04/28.
- Craig E, Bland R, Ndirangu J, Reilly JJ. Use of mid-upper arm circumference for determining overweight and overfatness in children and adolescents. Archives of disease in childhood. 2014;99(8):763-6. Epub 2014/06/04.
- Frisancho AR. New norms of upper limb fat and muscle areas for assessment of nutritional status. The American journal of clinical nutrition. 1981;34(11):2540-5. Epub 1981/11/01.
- Gartner A, Maire B, Kameli Y, Traissac P, Delpeuch F. Body composition unaltered for African women classified as 'normal but vulnerable' by body mass index and mid-upper-arm-circumference criteria. European journal of clinical nutrition. 2001;55(5):393-9. Epub 2001/05/30.
- Heymsfield SB, McManus C, Smith J, Stevens V, Nixon DW. Anthropometric measurement of muscle mass: revised equations for calculating bone-free arm muscle area. The American journal of clinical nutrition. 1982;36(4):680-90. Epub 1982/10/01.
- Ismail SJ, Manandhar M. Better Nutrition for Older People: Assessment and Action. HelpAge International 1999.
- Jordao AA, Bellucci AD, Dutra de Oliveira JE, Sergio Marchini J. Midarm computerized tomography fat, muscle and total areas correlation with nutritional assessment data. International journal of obesity and related metabolic disorders : journal of the International Association for the Study of Obesity. 2004;28(11):1451-5. Epub 2004/09/10.
- Mazicioglu MM, Hatipoglu N, Ozturk A, Cicek B, Ustunbas HB, Kurtoglu S. Waist circumference and mid-upper arm circumference in evaluation of obesity in children aged between 6 and 17 years. Journal of clinical research in pediatric endocrinology. 2010;2(4):144-50. Epub 2011/01/29.
- Reilly JJ. Mid-upper arm circumference (MUAC): new applications for an old measure. Archives of disease in childhood. 2017;102(1):1-2. Epub 2016/11/11
- Tsai AC, Chang TL, Yang TW, Chang-Lee SN, Tsay SF. A modified mini nutritional assessment without BMI predicts nutritional status of community-living elderly in Taiwan. The journal of nutrition, health & aging. 2010;14(3):183-9. Epub 2010/03/02.
- http://www.who.int/bulletin/volumes/90/12/12-109009/en/
- https://www.who.int/tools/child-growth-standards/standards/arm-circumference-for-age
- http://www.bapen.org.uk/pdfs/must/must_page6.pdf
- http://motherchildnutrition.org/early-malnutrition-detection/detection-referral-children-with-acute-malnutrition/muac.htm
- https://www.who.int/publications/i/item/9789241598163
- http://apps.who.int/iris/bitstream/10665/119207/1/emhj_2002_8_4_5_612_618.pdf
